Muscle testing is a crucial procedure used in clinical settings to assess muscular strength and function, playing a pivotal role in diagnosing, evaluating, and managing various neuromuscular conditions. In this comprehensive blog post, we’ll dive into the muscle testing grading system and the criteria for each grade. We aim to present this complex topic in a reader-friendly manner, catering to both healthcare professionals and general readers.
About Muscle Testing

Muscle testing, also known as manual muscle testing (MMT), is a common practice in physical therapy and neurology. Here, we’ll delve into its basics, its history, and its primary objectives.
The Basics
Muscle testing refers to a procedure used to evaluate the functional status of muscles. This test is critical for assessing motor function and diagnosing potential neuromuscular disorders. A well-performed muscle test can help identify weakness, measure progress, guide treatment, and predict outcomes.
- Identification of Weakness: Clinicians use MMT to spot muscle weakness that could result from a neurological condition, muscle disease, or a structural defect.
- Measure Progress: MMT serves as a tool to measure a patient’s progress during rehabilitation.
- Guide Treatment: It can guide the planning and modification of therapeutic strategies.
- Predict Outcomes: The severity of muscle weakness often correlates with prognosis, aiding in the prediction of functional outcomes.
History and Objectives
The roots of muscle testing trace back to the early 20th century, when clinicians started evaluating muscle strength manually. The goal was to quantify muscle strength in a standardized and reproducible manner. As time went on, muscle testing evolved, and it’s now an indispensable tool in the assessment and management of neuromuscular conditions.
- Standardization: This was a pivotal turning point in the development of MMT, allowing for consistency across assessments.
- Reproducibility: With standardization came reproducibility, allowing different clinicians to assess muscle strength and achieve similar results.
- Diagnosis and Management: MMT is used to diagnose various neurological and musculoskeletal conditions, track their progression, and manage treatment.
Grading System
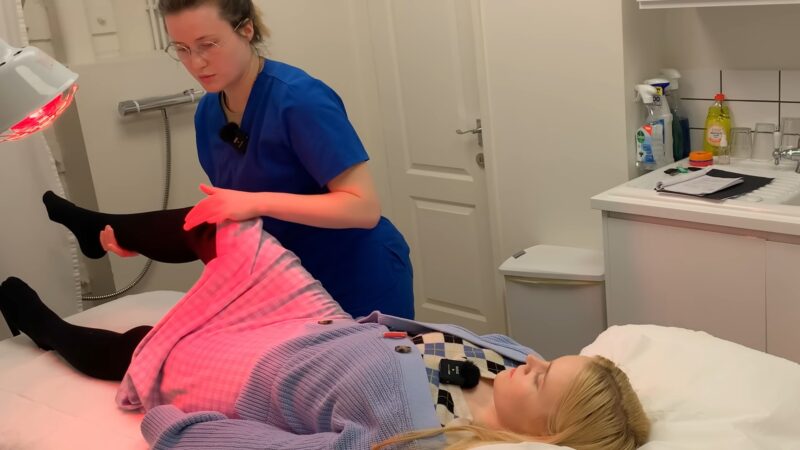
Next, we’ll dig deeper into the muscle testing grading system. This grading system ranges from 0 to 5, reflecting the muscle’s ability to resist gravity and applied pressure.
How It Works
The muscle testing grading system is based on the muscle’s ability to resist applied force in various positions. The grades range from 0 (no visible muscle contraction) to 5 (full strength against gravity and resistance).
- Grade 0: No visible or palpable muscle contraction.
- Grade 1: Visible or palpable muscle contraction but no joint movement.
- Grade 2: Ability to move the joint through its range in a gravity-eliminated position.
- Grade 3: Ability to move the joint through its range against gravity but not against resistance.
- Grade 4: Ability to move the joint through its range against gravity and some resistance, but less than normal.
- Grade 5: Ability to move the joint through its range against gravity and full resistance; this is considered normal muscle strength.
Variations and Specific Criteria
While the aforementioned grading scale is most commonly used, there are variations in practice. Some clinicians use a more detailed 10-point scale (0-10) for a more nuanced assessment. There’s also a +/- system used with the 0-5 scale to provide more detail (for instance, a grade of 4+ would indicate strength slightly less than normal but greater than a regular grade 4).
Also, it’s essential to note that muscle grading is based on specific criteria:
- Consistency: The muscle strength must be consistent across multiple tests.
- Patient’s Effort: The patient must give a maximal effort during the test.
- Appropriate Positioning: The positioning of the patient and therapist must allow for optimal muscle function.
- Correct Application of Resistance: The therapist should apply resistance in a direction opposite to the muscle’s action.
Clinical Significance and Limitations
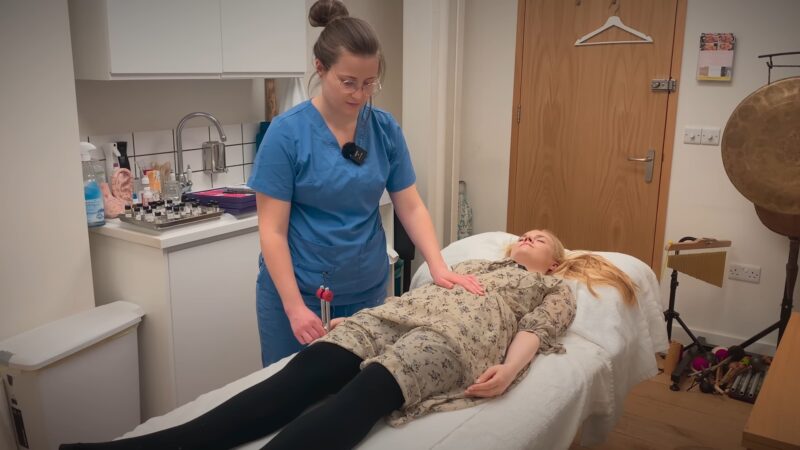
Muscle testing provides essential insights into the functional status of muscles, but it’s not without limitations. In this section, we’ll look at its clinical significance and explore its limitations.
Clinical Significance
Muscle testing provides clinicians with a quick and easy way to assess a patient’s muscle strength. This can be a game changer in diagnosing and managing conditions such as stroke, muscular dystrophy, peripheral neuropathy, and spinal cord injury, to name a few. MMT also has prognostic value, helping therapists predict outcomes and guide therapeutic strategies.
Limitations
While MMT is a valuable tool, it does have its limitations. It is subjective in nature, depending on the examiner’s skill and interpretation. It can also be affected by the patient’s effort, understanding, and cooperation. Furthermore, MMT may not accurately reflect functional abilities, especially in patients with higher muscle grades (4-5).
What Future Holds

Muscle testing continues to evolve, with new technologies and methodologies enhancing its efficacy and accuracy. As we look to the future, it’s clear that MMT will continue to be a key player in the assessment and management of neuromuscular conditions.
Technological Advancements
New technologies such as dynamometers and electromyography (EMG) are starting to supplement manual muscle testing. These devices provide more precise and objective measurements of muscle strength. The use of these technologies in conjunction with traditional MMT may lead to more accurate assessments and better patient outcomes.
New Methodologies
In addition to new technologies, innovative methodologies are enhancing muscle testing. Functional muscle testing, which evaluates muscles during functional tasks rather than in isolation, is gaining traction. This approach might provide a more accurate representation of a patient’s functional abilities.
Relevance in Different Medical Specialties
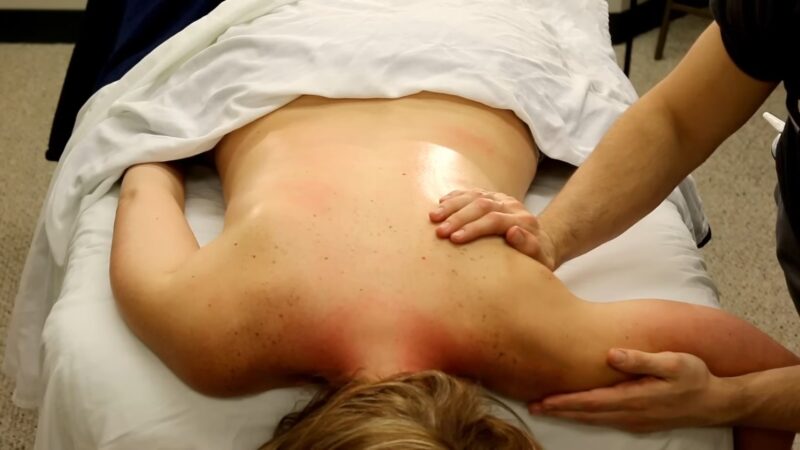
Beyond physical therapy and neurology, muscle testing plays a crucial role in multiple medical fields. Let’s delve into its significance in orthopedics, sports medicine, and occupational therapy.
In Orthopedics
In orthopedics, muscle testing is vital for diagnosing and treating conditions affecting the musculoskeletal system. It helps orthopedists to detect muscular imbalances and dysfunctions, which are often the culprits behind chronic pain and disability.
- Pre-operative Assessment: Muscle testing is used to evaluate the strength and function of muscles before surgical procedures, helping to plan the intervention and predict outcomes.
- Post-operative Rehabilitation: It is used post-operatively to track recovery and guide rehabilitation.
In Sports Medicine
In the world of sports medicine, muscle testing is key to athletic performance and injury prevention. A thorough muscle test can uncover weaknesses that may predispose an athlete to injury.
- Performance Optimization: By identifying areas of weakness, training programs can be tailored to enhance strength, power, and endurance, optimizing performance.
- Injury Prevention: Regular muscle testing can help catch potential issues early, allowing for corrective measures to be taken before an injury occurs.
In Occupational Therapy
Occupational therapists use muscle testing to evaluate and treat patients whose ability to perform daily activities is affected by muscle weakness.
- Assessment of Functional Ability: Muscle testing helps occupational therapists to assess the patient’s ability to perform tasks like lifting, carrying, or gripping and to develop a treatment plan accordingly.
- Task-specific Training: Based on muscle testing results, therapists can devise task-specific training programs to improve muscle strength and functionality, thus enhancing the patient’s quality of life.
Muscle Testing Across Different Age Groups
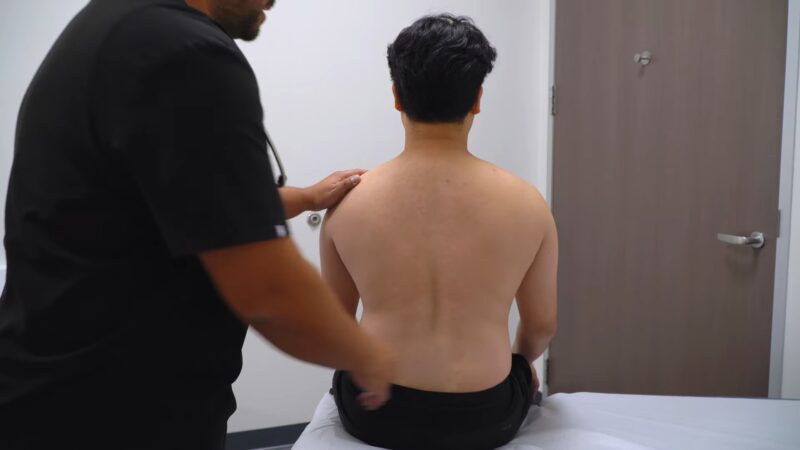
It’s worth noting that muscle testing has valuable applications across all age groups, from pediatrics to geriatrics. Here, we’ll examine the role of muscle testing in different age brackets.
In Pediatrics
In pediatrics, muscle testing aids in diagnosing and managing conditions like cerebral palsy, muscular dystrophy, and nerve injuries. A child’s muscle strength can significantly impact their motor development, and early detection of any issues can lead to timely interventions and better outcomes.
In Geriatrics
As we age, muscle strength naturally declines, often leading to mobility issues and increased fall risk. Regular muscle testing in the geriatric population can help identify early signs of muscle weakness, allowing for timely interventions and the potential to improve overall health and independence.
FAQs
Who can perform muscle testing?
Muscle strength evaluation may be performed by various practitioners, including nurses, physicians, physical therapists, occupational therapists, and chiropractors.
What is the most commonly accepted method of evaluating muscle strength?
The most commonly accepted method of evaluating muscle strength is the Medical Research Council (MRC) Manual Muscle Testing scale. This method involves testing key muscles from the upper and lower extremities against the examiner’s resistance and grading the patient’s strength on a 0 to 5 scale accordingly.
Which muscles are commonly tested?
Commonly tested muscles include the shoulder abductors, elbow flexors, elbow extensors, wrist extensors, finger flexors, hand intrinsics, hip flexors, knee extensors, dorsiflexors, great toe extensor, and plantar flexors.
What are the limitations of the MRC Manual Muscle Testing method?
Despite its advantages, the MRC method has its limitations. Scoring is subjective based on the examiner’s perception. There is variability between examiners for the maximal resistance they are able to apply.
The test does not account for musculoskeletal conditions that may make testing painful or difficult to tolerate. The test is dependent on patient effort, which may be poor in some patients. Finally, the grading system classifies strength level but does not directly quantify strength.
What are the alternatives to the MRC Manual Muscle Testing system?
Alternatives to the MRC system aim to quantify strength directly in terms of pounds, Newtons, or other units. This requires specialized equipment, most commonly dynamometers. Dynamometry provides a more precise measurement of the force that a muscle can exert and can allow for differences in strength to be tracked over time.
What is the clinical significance of muscle strength testing?
Muscle strength testing can help a practitioner diagnose neurologic problems in which weakness is a prominent deficit. The muscles targeted for testing should be methodically chosen based on suspected diagnoses and for complete characterization of the strength deficit in various limbs. Careful technique is important for ensuring valid and reproducible results.
Final Words
Muscle testing is an indispensable tool in physical therapy and neurology, aiding in the diagnosis and management of various neuromuscular conditions. Understanding the grading system and criteria for it is vital for both clinicians and patients alike. With new technologies and methodologies emerging, the future of muscle testing looks brighter than ever.

